Virginia Pain
Specialists
Nino M. Dobrovic, M.D.
Pain Management
There are many types of pain: neuropathic, nociceptive, visceral, somatic, and psychosomatic, to name a few. The types and their nomenclature vary widely, since pain is a very personal issue. Even within the healthcare community, there are variations in nomenclature and approach. However, all of these types of pain can be teased apart in an effort to understand and treat the causes of a patient's suffering. At VPS we primarily focus on spine related pain, as well as the more common neuropathic and nociceptive types of pain.
Spine Care
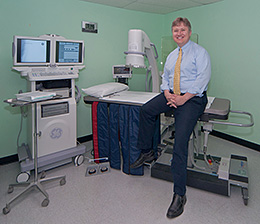
 At VPS, we have personal experience with pain from the spine. Dr. Dobrovic has a herniated disc, and as he puts it, "if I don't mind my Pilates, my disc talks to me with burning pain down the right leg into the heel." And yet, he downhill skis with his teenage sons whenever possible. In addition to this personal involvement and sympathy with our patients, Dr. Dobrovic is one of the few physicians to practice interventional pain management, by which we mean injections using fluoroscopy — an imaging technology commonly used by physicians to obtain real-time moving images of the internal structures of a patient. This allows highly targeted use of the injections to treat the locus of the pain source. This is a fantastic tool, but with limitations which are important for the physician to of which to stay cognizant.
At VPS, we have personal experience with pain from the spine. Dr. Dobrovic has a herniated disc, and as he puts it, "if I don't mind my Pilates, my disc talks to me with burning pain down the right leg into the heel." And yet, he downhill skis with his teenage sons whenever possible. In addition to this personal involvement and sympathy with our patients, Dr. Dobrovic is one of the few physicians to practice interventional pain management, by which we mean injections using fluoroscopy — an imaging technology commonly used by physicians to obtain real-time moving images of the internal structures of a patient. This allows highly targeted use of the injections to treat the locus of the pain source. This is a fantastic tool, but with limitations which are important for the physician to of which to stay cognizant.
Spine Pain Generators
- discs
- facets
- muscles (most likely as a result of issues with disc(s), but non-radiating)
- nerves (if in a radiating pattern)
- sacroiliac joint
Diagnosing and treating spine pain requires an exceptional knowledge of anatomy, an excellent history from the patient, and clear physical findings. Sometimes the results are not clear, but the majority of cases are, and the results can be very satisfying both for the patient and the physician. This is a process, not a sudden magical cure. It starts with a diagnosis, then, if appropriate, a well-placed injection with the assistance of the fluoroscopy suite, and feedback from the honest patient — part of where the collaborative teamwork between the patient and physician that is critically important in pain management. This results in finding a treatable pain generator, which means what was just described is the beginning of this treatment regimen when found to be appropriate.
Health & Wellness
An ongoing theme in the treatment of pain is health and wellness. For spine pain, a health maintenance program will be a likely part of your collaborative treatment — your homework, if you wish. Aquatics, yoga, and (Dr. Dobrovic's favorite) Pilates are some examples of the tools you may need to make part of your life to help your body heal and to reduce the possibility or severity of recurrence. All of us, but especially those on a regimen of treatment for pain, must embrace lifelong maintenance of our bodies in good health.
Managing Our Expectations
You are here for relief from or amelioration of pain. Once anyone experiences severe and/or intractable pain, one of the common emotional responses is hypersensitivity to pain, from the fear that the extreme pain will return. For some, this turns the ordinary, common, everyday pain into red flags of impending crises. Part of your treatment will be to help you understand the separation of pain that needs treatment, the degree to which a given diagnosis can likely be treated, and recognized the ebbs and flows of pain from the ordinary process of living. This is all part of our collaboration, in which Dr. Dobrovic will help you gain the best outcome possible and return to the most vital, full life possible.
Neuropathic Pain
Neuropathic pain may arise as a consequence of a lesion or disease affecting the receptors and processing centres that produce the senses such as touch, temperature, proprioception (body position), and nociception (pain). It may be associated with abnormal sensations called dysesthesia, which occur spontaneously and allodynia that occurs in response to external stimuli. Neuropathic pain may have continuous and/or episodic (paroxysmal) components. The latter are likened to an electric shock. Common qualities include burning or coldness, "pins and needles" sensations, numbness and itching.
- shingles
- crush injuries
- CRPS (complex regional pain syndrome)
- radiculopathy
- cancer (frequently irradiation therapy and/or chemotherapy)
Central neuropathic pain is found in spinal cord injury, multiple sclerosis, and some strokes. Fibromyalgia, a disorder of chronic widespread pain, is potentially a central pain disorder and is responsive to medications that are effective for neuropathic pain.
Aside from diabetes and other metabolic conditions, the common causes of painful peripheral neuropathies are herpes zoster infection, HIV-related neuropathies, nutritional deficiencies, toxins, remote manifestations of malignancies, genetic, and immune mediated disorders or physical trauma to a nerve trunk.
Neuropathic pain is common in cancer as a direct result of cancer on peripheral nerves, e.g., compression by a tumor, or as a side effect of chemotherapy, radiation injury or surgery.
How Do We Treat Neuropathic Pain?
Occasional injections can ameliorate, as can a managed polypharmaceutical regimen. Managed polypharmacy does take time, and with results that are good, but not often dramatic. A dorsal column stimulator trial may provide some relief. We can work together to address how the pain affects your life, your mood, sleep patterns, general functionality, and provide relief by behavioral modification. Exercise often helps to at least ameliorate such pain.
Nociceptive pain
Nociceptive pain is more commonly described as aching. Nociceptive pain is caused by stimulation of peripheral nerve fibers (nociceptors) that respond only to stimuli approaching or exceeding harmful intensity, and may be classified according to the mode of noxious stimulation; the most common categories being "thermal" (heat or cold), "mechanical" (crushing, tearing, etc.) and "chemical" (iodine in a cut, chili powder in the eyes).
- osteoarthritis
- acute pain, e.g., post-surgical pain
- cancer (active lesions)
Nociceptive pain may also be divided into "visceral," "deep somatic," and "superficial somatic" pain. Visceral pain originates in the viscera (organs) and often is extremely difficult to locate, and nociception from some visceral regions produces "referred" pain, where the sensation is located in an area distant from the site of the stimulus. Deep somatic pain is initiated by stimulation of nociceptors in ligaments, tendons, bones, blood vessels, fasciae and muscles, and is dull, aching, poorly-localized pain. Examples include sprains and broken bones. Superficial pain is initiated by activation of nociceptors in the skin or superficial tissues, and is sharp, well-defined and clearly located. Examples of injuries that produce superficial somatic pain include minor wounds and minor (first degree) burns.
The classic example of nociceptive pain is an acute injury, such as a stubbed toe. It gets your attention at least to look at it and tend to it. You may have broken a bone. The body's response to an injury is not only with pain, but an entire symphony of responses. Such event-driven pain responds well to ice, rest. immobilization, anti-inflammatories, rest, and you know it will get better with a tincture of time. Usually, you don't visit a physician with such a pain, unless it persists or there is evidence of something extreme, such as a clear break that needs setting or other treatment.
Nociceptive pain may also be chronic, as with someone with a "bad knee." Usually, there was some event that "disrupted the normal tissue in a variety of possible ways. Whatever happened to whatever part of the body, the resultant complaint is that there is pain when used, pressed, twisted, etc. There may or may not be evidence with swelling or redness, there may or may not be scars or other attendant "aha!" sources of clarity. There may be simply arthritis or RA.
How Do We Treat Nociceptive Pain?
All such patients need conservative care. They may be too young for a hip replacement, for example. NSAIDs, such as ibuprofen, can be an approach, but they have the limitation of GI and renal toxicity over time. Bracing, activity modification, and opioids, which carry risk and responsibility for both the patient and the physician. Topical NSAIDs are an emerging bright spot for such treatment. Ultimately, nociceptive pain is common, is activity and/or use (of that body part) based, and can be resolved if the "offending" tissue is addressed.
What Makes VPS Different?
Some of this will seems counter intuitive, because you will think that every physician does what I will describe, but sadly, that is not so.
First, I will examine you carefully and in depth. This won't be a assistant, or a third party, and I will verify your medical history, and we will talk about your difficulty and you will tell me about it and I will listen. After this, and the results from lab tests, I will provide you with either
- a diagnosis, which means a specific determination of what I think is the source of your pain, or
- a differential diagnosis, which is medical speak for a list of possible sources of your pain, which means the source or your pain is (somewhat) ambiguous or not sufficiently clearly delineated to pick one or rule out others. This is common, and a result of the fact that our bodies don't read medical texts and fit themselves neatly into the finite responses and categories written therein.
We will discuss the findings so that you understand them as much as possible.
At this point, I will perform reasonably priced medical procedures that I know to be specific to the diagnosis. One of the differences of my practice is that I do not try to enrich myself at your expense by pushing on you unnecessary and ineffective, but accepted, costly procedures. This is not true for many practitioners. As I have said and will continue to say, your treatment at VPS with me, is collaborative and all about you.
Page Contents
![]()
Spine Conditions
- Annular Tear
- Arthritis of the Spine
- Bone Spurs
- Bulging Disc
- Canal Stenosis
- Degenerative Disc Disease
- Degenerative Spine
- Disc Protrusion
- Facet Disease
- Failed Back Surgery Syndrome
- Foraminal Stenosis
- Herniated Disc
- Herniated Nucleus Pulposus (HNP)
- Pinched Nerve
- Prolapsed Disc
- Ruptured Disc
- Sciatica
- Slipped Disc
- Spinal Stenosis
- Spondylitis
- Spondylolisthesis
- Spondylosis